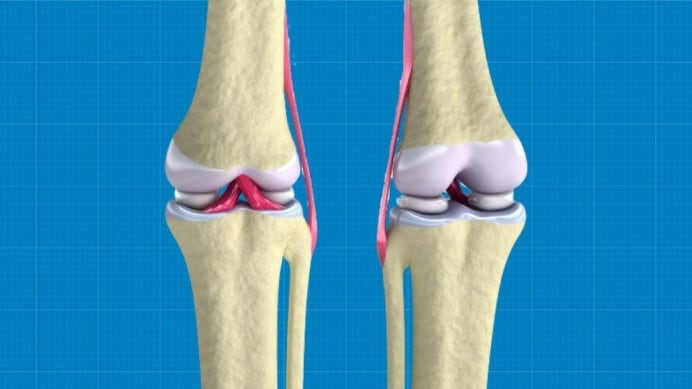
Scientists 3D-Bioprint Regenerative Knee Cartilage Tissue
The tissue could easily help those suffering from arthritis or other knee injuries.
Our knees are notoriously famous for getting injured, or simply deteriorating with age. The aches and pains that come from them can be excruciating and turn a simple action, such as walking, into a painful one.
So it’s no wonder scientists have been working on creating 3D hybrid bioinks that can 3D print structures to replace damaged knee cartilage.
Researchers from the Wake Forest Institute for Regenerative Medicine (WFIRM) have been working on a proof-of-concept study, which looks into a new method for 3D bioprinting. This 3D printing creates cartilage and supporting structures that can be used as a replacement of damaged meniscus — the rubbery cartilage in your knee.
The study was published in Chemistry of Materials in late September.
Our meniscus is at risk of being damaged from sports injuries or just from age-related wearing out. This cartilage acts as a cushion between the upper and lower leg bones from rubbing against one another, so when it disappears or is worn down, these bones grind together in a rather unpleasant manner.
The WFIRM team used a number of different bioinks together so as to 3D print the complete fibrocartilage tissue layer by layer. The first layer encourages the body’s cells to repopulate, and the second keeps the structure strong and flexible.
“In this study, we have been able to produce a highly elastic hybrid construct for advanced fibrocartilaginous regeneration,” said Sang Jin Lee, associate professor at WFIRM and author of the study.
“The results demonstrate that this bioprinted construct offers a versatile and promising alternative for the production of this type of tissue.”
The structure has been tested out on mice, and 10 weeksafter surgery these mice began to regenerate their own fibrocartilage.
Further tests and studies need to be carried out by the team so as to monitor the body’s responses to the implant, and to see whether a human body would show the same results as those found in mice.
Anthony Atala, director of WFIRM, explained, “This proof-of-concept study helps point our work in the right direction to someday be able to engineer this crucial tissue that is so important for patients.”
Source:https://interestingengineering.com